- CAGD President Dr. Howard Chi shares the core values of the AGD
- 2016 CAGD annual meeting held at the Fairmont Hotel in Newport Beach
in January - The CAGD Hands-on Experience: Implant hands-on is very close to reality
- The learning potentials in your neighborhood
I-Integrating Implant Dentistry into General Practice
II- One-piece Dental Implant Placement in Narrow Ridges/Spaces - CAGD’s GP News (printed magazine, March 2016 issue)
is now available online
CAGD President Dr. Howard Chi shares the core values of the AGD
CAGD President Dr. Howard Chi shares the core values of the AGD and the current issues facing general dentistry.

2016 CAGD annual meeting held at the Fairmont Hotel in Newport Beach
in January




The CAGD Hands-on Experience: Implant hands-on is very close to reality
Lots of tools and lots of fun with Dr. Mike Chen’s Handson course at the CAGD annual meeting on January 30, 2016
The learning potentials in your neighborhood
I-Integrating Implant Dentistry into General Practice
II- One-piece Dental Implant Placement in Narrow Ridges/Spaces
Belonging to a local community of dentists that is based on the foundation of sharing knowledge is one of the best learning experiences we can encounter. At a recent study club meeting in Davis in Northern CA organized by the SacramentoSierra AGD and the Davis Dental Institute, a group of local dentists shared some of the newest dental implant related procedures in their practices. The presenters humbly acknowledged that they should not be considered “a high authority” on these topics, they are just simply sharing what they do in their practices.
I-Integrating Implant Dentistry into General Practice:
Increasing Predictability and Success Rate of Implant Placement
Presented by James W. Childress, DDS, FIOCI
Private General Dental Practice, Davis, CA
clientuploads/Potentials 1.jpg
Dr. Childress presenting
“Integrating Implant Dentistry into General Practice”
Atrophied ridges under bridge pontics, the challenge of restoring less than ideally placed implants, and the greater chance of success when a case is planned with the final prosthetic result in mind are among the reasons Dr. Childress decided to start placing dental implants in his practice. He cited Yogi Berra, “If you don’t know where you are going you will wind up someplace else.”
Some of the key elements Dr. Childress stressed on to increase the predictability and the success rate of implant placement were:

- Training: A GPR residency and 35 years of surgical experience did not hinder Dr. Childress from seeking over 200 hours of continuing education in the past 3 years. He attended socket presentation, guided bone regeneration, implant placement, and soft tissue management courses including hands-on implant surgery in study clubs where an instructor was dedicated to guiding attendees during live surgeries on their own patients.
- CBCT in your own practice: Patients then don’t need to travel, and are able to get the procedure started quickly. Patients also recognize improved technology, safety, and predictability.
- Utilizing Surgical Guides: Computer-generated surgical guides should be utilized for all cases. They have many advantages. They ensure proper angulations and depth of implants, decrease surgery time, keep osteotomy burs on course when fully guided, and eliminate drifting to softer bone. Surgical guides also have disadvantages including their high cost, very challenging with limited openings, sometimes need to insert bur into the guide and bring to mouth as one unit. Surgical guides can be trusted, but still need to be verified in the mouth first.
- Support: Colleagues and family support is invaluable. Integrating implant dentistry into general practice requires considerable time and financial investment.
- Keeping up with newest technology: Adding concentrated growth factors from the patients’ own blood (L-PRF) to grafting protocol speeds healing and new bone formation and seems to lower postop pain.
- Scheduling factors: No double booking, schedule plenty of time, complete hygiene checks prior to surgery, have a second assistant at all times standing by.
- Strict protocol for sterile environment and technique.
- Antibiotic coverage: For non infected sites, Rx Amoxicillin 2 grams 1 hour prior + 500mg TID x 5days. For infected sites, Rx Clindamycin 150mg TID x 5days prior to procedure + 5days after. Do not graft if pus is present, extract and wait 3-4 weeks.
Case presentation:
78 year old presented with pain on biting. Examination of #12 revealed a split tooth and a very loose buccal tooth segment indicative of a horizontal midroot fracture (Fig. 1). Upon removal of the tooth, a fracture of the buccal plate as well as the buccal midroot were noted explaining the looseness of the buccal tooth segment (Fig. 2,3).
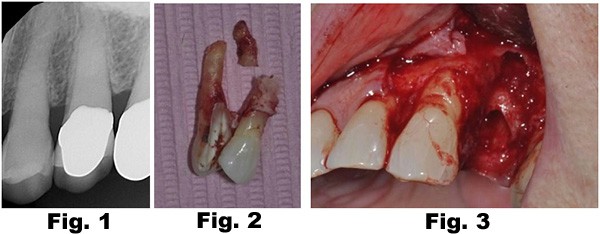
A bone graft was placed (Fig 4), covered with a PTFE non-resorbable membrane and secured with PTFE sutures Fig. 5). The sutures can be removed 2-3 weeks postop and the membrane can be removed 4-6 weeks post-op (Fig. 6).
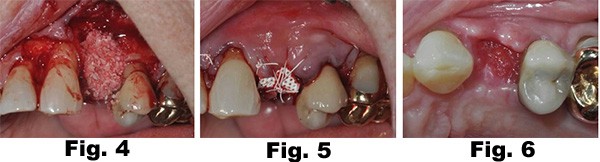
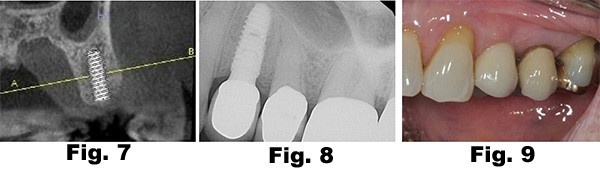
Implant placement was planned using a CBCT (Fig. 7). The implant was placed and was restored with a custom abutment and a PFM crown 6 months after implant placement (Fig. 8,9)
II- One-piece dental implant placement for narrow ridges/spaces
Presented by Vahid Farahyar, DDS, AF AAID
Private General Dental Practice, Davis, CA
clientuploads/One Piece.jpg
Dr. Farahyar presenting
“One-Piece Dental Implants”

One-Piece Dental Implants (OPI) are a great option worthy of consideration to replace single missing teeth in narrow ridges and spaces. Dr. Farahyar shared the knowledge he acquired throughout the years by attending didactic and handson continuing education courses, reading text books and articles, and form firsthand experience with OPIs including indications, advantages, disadvantages, and techniques.
Dental implants should be at least 1.5 mm away from the adjacent teeth, at least 3 mm away from an adjacent implant, and >1 mm of bone should be present on the facial and lingual of the implant.
In order to maintain 1.5 mm between an implant and its adjacent teeth in an edentulous area with 6 mm of interdental space, a 3 mm onepiece dental implant can be placed.
OPIs have many advantages:
- OPIs have increased mechanical strength due to the unified structure of the implant and the abutment
- OPIs require less surgical procedures and prosthetic components
- OPIs show reduced marginal bone loss as they lacks the microgap between the implant and the abutment, thus eliminating the micromovent of the abutment and the harboring of bacteria
- There is no loosening or fracturing of an abutment screw (healing abutment or prosthetic abutment)
- Many OPIs follow the conventional crown and bridge procedure: preparation, temporization, impression, and cementation
However, they also have disadvantages:
- The implant angulation must be ideal as it is not possible to correct the abutment angle significantly
- The implant abutment is not versatile (for instance, an abutment of a twopiece design may be changed from a ball attachment to a conventional crown abutment to accommodate a change from a removable to a fixed prosthesis or vice versa)
- It should not be used in posterior edentulous areas where the restoration is under immediate heavy occlusal load
- OPIs require immediate restoration. This adds more chair time and may cause micromovement at the boneimplant interface which could lead to implant failure
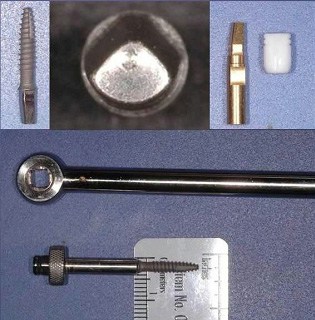
The technique that Dr. Farahyar follows while placing a 3mm one piece dental implant requires initiating an osteotomy with a 1.8 mm or smaller drill and finalizing it with a 2.3 mm drill. The implant is then inserted with a special insertion tool as seen in the figure to right. A temporary crown is placed after implant placement. After the implant osseointegrates, a regular crown impression of the onepiece dental implant can be made to fabricate the final restoration.
Case presentation:
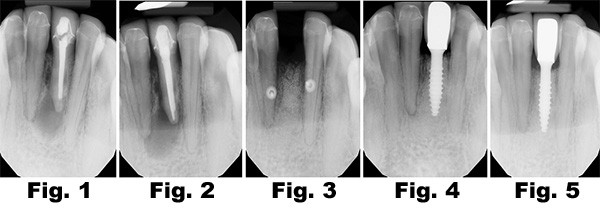
A patient presented with a PA lesion #24 (Fig. 1). The lesion showed progression 6 months after endodontic retreatment (Fig. 2). Tooth #24 was extracted, and a bone graft was placed and covered with a resorbable membrane and primary soft tissue closure (Fig. 3). A onepiece dental implant was placed and was restored 8 months after implant placement (Fig. 4). Figure 5 demonstrates successful implant osseointegration and restoration 6 months post placing the restoration.
CAGD’s GP News (printed magazine, March 2016 issue) is now available online
The GP News features clinical articles, upcoming
and past CE course details, advocacy updates, news
and events of the CAGD, local components, and
student Fellowship tracks at all California dental
schools


